Quick safety note: This article is general education, not personal medical advice. If you have chest pain, trouble breathing, fainting, new weakness on one side, facial droop, speech trouble, or symptoms that feel “different/worse than usual,” call emergency services right away.
AFib (atrial fibrillation) has a talent for showing up uninvitedlike that friend who “just happened to be nearby” and also “just happened” to finish your snacks. The good news: while you can’t always control every episode, you can absolutely make AFib’s job harder. Think of prevention as removing the welcome mat, changing the locks, and installing a motion sensor light that screams, “NOT TODAY.”
AFib Prevention, in Plain English
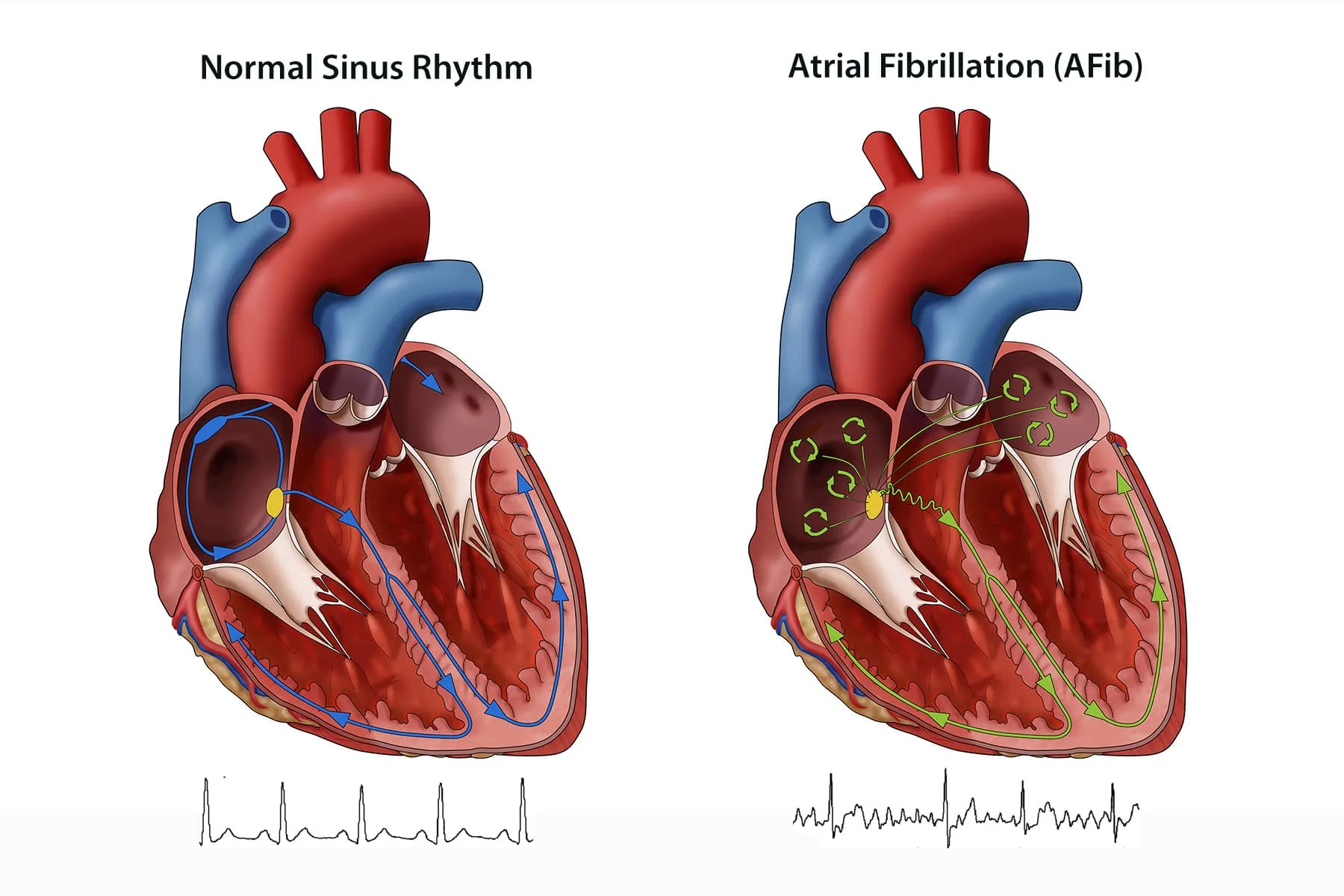
An “AFib attack” usually means an episode where your heart’s upper chambers (atria) beat in a chaotic, irregular pattern. Some people feel palpitations, fluttering, fatigue, shortness of breath, or dizziness. Others feel… basically nothing (which is both convenient and annoying). Prevention has two layers:
- Long-game prevention: Reduce how often episodes happen and how long they last by addressing triggers and risk factors.
- Right-now prevention: If you feel an episode coming on, use a calm, structured plan to avoid escalating itand know when it’s time to get help.
Step 1: Learn Your AFib “Triggers” (Because AFib Loves Patterns)
Triggers are the spark; risk factors are the pile of dry leaves. Your goal is to remove both. A practical way to start: keep a simple “AFib receipt” log for 2–4 weekssleep, alcohol, caffeine, stress, illness, big meals, workouts, dehydration, and any new meds/supplements.
Common AFib Triggers to Watch For
- Alcohol (especially binge drinking): For many people, it’s a top trigger. If your AFib tends to “party,” alcohol is often the DJ.
- Dehydration and electrolyte dips: Not glamorous, but very realespecially after sweating, vomiting/diarrhea, long flights, or “I forgot water exists” days.
- Stimulants: Some cold/allergy meds, energy drinks, certain supplements, and recreational drugs can push your heart rhythm the wrong way.
- Poor sleep / sleep apnea: Bad sleep can raise your risk and make episodes more likelysnoring isn’t always “just snoring.”
- Stress and adrenaline spikes: Work emergencies, arguments, panic, even exciting events can be a trigger for some people.
- Illness and inflammation: Viral infections, fever, and post-surgery stress can set off episodes.
- Heavy meals (especially salty or ultra-processed): Some people notice symptoms after large late dinnersyour heart dislikes surprise midnight buffets.
- Exercisetoo little or too intense: Regular movement helps, but sudden “hero workouts” after weeks of couch life can backfire.
A Simple Trigger-Tracking Template
When symptoms happen, jot down:
- Time + duration
- What you were doing 1–6 hours before
- Sleep quality (0–10)
- Alcohol/caffeine (type + amount)
- Hydration (roughly how much water)
- Stress level (0–10)
- Any illness, new meds, or supplements
Bring this to your clinician. It turns “I think it’s random” into “Here’s the pattern.” AFib hates receipts.
Step 2: Make Lifestyle Changes That Actually Move the Needle
Not all lifestyle advice is created equal. “Just relax” is not a plan. The best AFib-prevention habits are the ones that address the drivers of AFib: blood pressure, weight, sleep, alcohol, fitness, smoking, and underlying conditions.
1) Treat Risk Factors Like They’re Part of the Rhythm Plan
AFib is strongly tied to common health conditions. If you’re treating AFib but ignoring blood pressure, sleep apnea, thyroid issues, or diabetes, it’s like mopping the floor while the sink is still overflowing.
- Blood pressure: Keep it in your target range (your clinician can set this). High BP is one of the biggest AFib accelerators.
- Weight management: Even modest, steady weight loss (when needed) can reduce AFib burden over time.
- Sleep apnea screening and treatment: If you snore, wake up unrefreshed, or feel sleepy during the day, get evaluated. Treating sleep apnea can improve AFib control for many people.
- Thyroid health: Overactive thyroid can trigger AFib; make sure yours is monitored if you’re at risk.
- Diabetes and cholesterol: Managing these supports heart health and reduces long-term complications.
2) Move Your BodyBut Don’t Ambush Your Heart
Regular, moderate-to-vigorous activity can reduce AFib burden and improves blood pressure, weight, sleep, and stress. The key is consistency, not intensity theater.
Try this “boring but powerful” approach:
- Start: 10–20 minutes of brisk walking most days.
- Build: Add 5 minutes every week or two until you’re consistently active.
- Add strength training: 2 days/week (light-to-moderate), focusing on form and breathing.
If your AFib is exercise-triggered or you have heart disease, ask your clinician for safe boundaries (heart-rate goals, warning signs, and whether cardiac rehab makes sense).
3) Alcohol: The “Dose Matters” Trigger (And Sometimes Zero Is the Move)
Many people with AFib notice episodes after drinking, especially with heavier intake. If AFib episodes are frequent, reducing alcoholor taking a break entirely for a few weekscan be an eye-opening experiment. If your episodes drop dramatically, you just found a big lever.
4) Caffeine: Personalize It (Don’t Assume Coffee Is Your Villain)
Caffeine is complicated: some people are sensitive, others are not. A helpful rule: if caffeine reliably triggers symptoms for you, treat it like a trigger; if it doesn’t, keep it moderate and consistent. Avoid “surprise caffeine”the triple espresso when you normally drink half-caf.
5) Hydration and Electrolytes: The Unsexy Superpower
Dehydration can raise your heart rate and make your rhythm more irritable. Aim for steady hydration (especially with heat, travel, or exercise). If you’ve had vomiting/diarrhea or heavy sweating, ask your clinician what electrolyte replacement is safe for youparticularly if you have kidney or heart failure concerns where fluid balance matters.
6) Sleep: Protect It Like It’s a Medication
AFib and poor sleep are frequent troublemakers together. Build a sleep routine that’s realistic:
- Keep a consistent wake time (even on weekends, within reason).
- Cut alcohol close to bedtime (it fragments sleep and can trigger AFib).
- Limit big late meals if they worsen symptoms.
- Get evaluated for sleep apnea if you snore or feel persistently tired.
7) Stress: Don’t “Eliminate” ItOutskill It
No one can delete stress. But you can change your nervous system’s reaction so your heart doesn’t feel like it’s sprinting from a bear when the bear is just an email.
- Micro-reset breathing: Inhale gently through the nose, exhale longer than you inhale, repeat 5–10 cycles.
- Daily decompression: 10 minutes of walking, stretching, or quiet timescheduled like a meeting.
- Reduce “stimulant stacking”: Poor sleep + caffeine + stress is a classic AFib combo meal.
Step 3: Take Medications Exactly as Prescribed (Yes, This Counts as Prevention)
This is where prevention becomes very un-funny: AFib can raise stroke risk, and medications are often the most direct way to lower that risk. If you’ve been prescribed:
- Blood thinners (anticoagulants): These help prevent clots that can cause stroke.
- Rate-control meds: Help keep your heart rate from racing during episodes.
- Rhythm-control meds: Help maintain normal rhythm or reduce episodes.
Take them as directed and talk to your clinician before stopping or changing anything. If side effects are an issue, don’t “rage-quit” the prescriptionask for options. There are usually alternatives.
Step 4: Have an “Uh-Oh, It’s Starting” Plan
If you feel symptoms like fluttering, racing, or irregular beats, your goal is to stay calm, gather information, and avoid making things worse. Here’s a general, low-risk checklist (unless your clinician has given you a specific action plan that overrides this):
The 10-Minute AFib Calm-Down Protocol
- Stop what you’re doing and sit down. No heroic stair sprints.
- Slow your breathing (longer exhales) and relax your shoulders/jaw.
- Check your pulse or wearable and note the time symptoms started.
- Hydrate with water (unless you’ve been told to restrict fluids).
- Avoid stimulants (caffeine, nicotine, energy drinks) and avoid alcohol.
- Use your prescribed “as-needed” plan if your clinician has given one.
- Reassess symptoms after 10–20 minutes: better, worse, or same?
Important: Don’t try random internet “maneuvers” or supplements to “shock” your rhythm back. AFib management is individualized, and some tactics used for other arrhythmias aren’t appropriate for AFib.
Step 5: Know When It’s Not a DIY Moment
Get urgent medical help if you have any of the following:
- Chest pain/pressure, severe shortness of breath, fainting, or near-fainting
- Signs of stroke (face drooping, arm weakness, speech trouble, sudden confusion, vision loss)
- New, intense symptoms or a heart rate that’s very fast with significant dizziness or weakness
- An AFib episode that lasts longer than your clinician’s guidance for you, especially if you’re not on a clear plan
Step 6: Ask About Longer-Term Options If Episodes Keep Happening
If you’re doing “all the right things” and AFib is still frequent or disruptive, that’s not a personal failureit’s a sign to revisit your strategy. Depending on your situation, your clinician may discuss:
- Early rhythm-control strategies to reduce burden and symptoms
- Cardioversion (restoring rhythm with a controlled electrical shock)
- Catheter ablation (targeting the tissue that triggers abnormal signals)
- Evaluating stroke-risk prevention strategies and adjusting anticoagulation when appropriate
AFib care is not one-size-fits-all. The best plan is the one you can sustainand the one that matches your AFib type, symptoms, and risk profile.
Putting It All Together: Your AFib Prevention “Starter Pack”
Daily (10–30 minutes total)
- Move: walk, bike, swim, or a simple home routine
- Hydrate steadily
- Take meds as prescribed
- One stress reset (breathing, short walk, stretching)
Weekly
- Plan meals that support blood pressure and weight goals
- Limit alcohol (or take a break and see what changes)
- Review your trigger log
- Strength training 2 days/week (as tolerated)
Monthly
- Check in on blood pressure trends
- Update your clinician with patterns: triggers, frequency, duration, symptoms
- Revisit sleep quality and possible sleep apnea screening if relevant
Conclusion
Preventing an AFib attack is less about finding one magical trick and more about stacking small advantages: consistent movement, solid sleep, smart hydration, fewer triggers, better control of blood pressure and weight, and taking medications correctly. You’re not trying to “win” against your heartyou’re trying to make your heart’s environment calmer, steadier, and less trigger-friendly.
And when AFib does try to crash the party anyway, you’ll have a plan, a log, and the confidence to know whether you should breathe, hydrate, and monitoror call for help. That’s real prevention: fewer surprises, fewer spirals, and more control.
Real-World Experiences: What People Learn While Trying to Prevent AFib Episodes (About )
People living with AFib often say the most frustrating part isn’t the episode itselfit’s the “Why now?” mystery. Over time, many discover AFib isn’t always random; it’s often picky. Here are a few common, real-world patterns people report as they learn to prevent episodes (shared here as typical experiences, not medical guarantees).
The “I Was Being Healthy… Mostly” Wake-Up Call
One common story goes like this: someone cleans up their diet, starts walking, and feels prouduntil AFib shows up anyway. When they look closer, the pattern is hiding in plain sight: inconsistent sleep, high stress, and “just one” energy drink on the busiest days. The lesson isn’t that healthy habits don’t work; it’s that AFib often reacts to clusters. A single trigger might not do much, but three triggers at once (bad sleep + stress + stimulants) can be enough to flip the switch.
The “Hydration Is Not Optional” Discovery
Many people learn the hard way that dehydration isn’t just about feeling thirsty. Episodes often show up after long flights, hot weather, intense yard work, or a stomach bug. Once people start treating hydration like a daily routinewater spaced throughout the day, plus extra fluids around exercisesome notice fewer “out of nowhere” flares. The funny part? Plenty of folks say they used to treat water like a decorative beverage, something you keep near you for good vibes. AFib does not respect vibes; it respects steady fluid balance.
The Alcohol Experiment That Changes Everything
Another frequent experience: someone doesn’t think alcohol is a factor because they’re not “a heavy drinker.” Then they try a 30-day break, and episodes drop. Or they notice a consistent pattern: AFib the night of drinking, or the next morning after poor sleep. For some, even moderate intake can be a trigger; for others, it’s only binge drinking. The point is personalizationyour trigger threshold may be very different from your friend’s.
Sleep Apnea: The Plot Twist
A lot of people are surprised when sleep apnea enters the chat. They weren’t coming to the doctor for snoringthey came for palpitations. After evaluation and treatment, some report fewer episodes, better energy, and less “wired but tired” stress. Even when AFib doesn’t disappear, better sleep can make episodes easier to manage and recovery faster.
Control Feels Better Than Perfection
Finally, many people say the biggest shift is mental: moving from “AFib is happening to me” to “I have a playbook.” A simple trigger log, a calm-down protocol, medication consistency, and clear emergency rules can reduce feareven when episodes still happen occasionally. Prevention isn’t perfection; it’s fewer flare-ups, less chaos, and a lot more confidence.