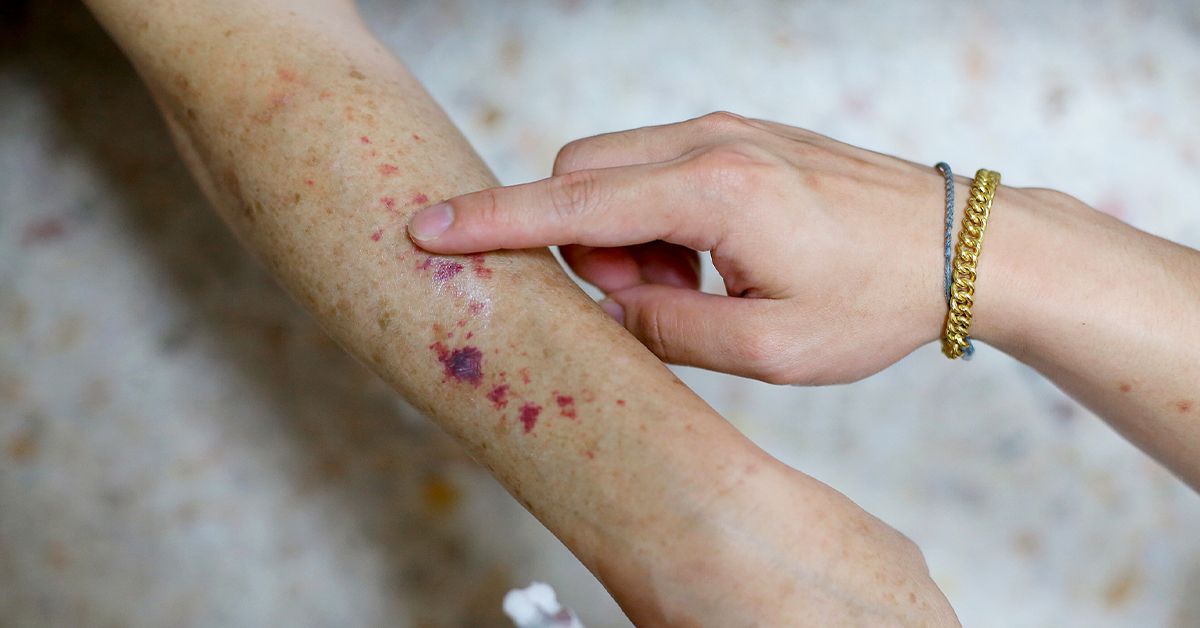
Tiny red or purple dots can send your brain into full detective mode fast. One minute you are brushing your teeth or getting dressed, and the next you are staring at your skin like it has started speaking in Morse code. Those little spots may be petechiae, and while the name sounds fancy, the basic idea is pretty simple: tiny blood vessels have leaked a small amount of blood under the skin or inside a mucous membrane.
The tricky part is that petechiae live in two very different worlds. In one world, they can show up after intense coughing, vomiting, heavy lifting, or minor friction and fade without drama. In the other world, they can be a clue to something that needs medical attention, such as a platelet problem, a medication side effect, an infection, or inflammation in the blood vessels. That is why petechiae are worth understanding. Your skin is not trying to be dramatic. It is trying to leave a note.
What Are Petechiae?
Petechiae are tiny, flat spots caused by bleeding under the skin. They are usually pinpoint-sized and may look red, purple, or brown depending on your skin tone. They are not raised, they do not feel like bumps, and they do not turn white when you press on them. That last detail matters because many ordinary rashes blanch, but petechiae usually do not.
Petechiae can appear almost anywhere, including the legs, arms, chest, stomach, inside the mouth, on the eyelids, or even in the whites of the eyes. Sometimes they stay as scattered pinpoints. Sometimes they cluster and look rash-like, which is why people often mistake them for irritation, heat rash, or allergy spots at first glance.
They also sit on a spectrum with two related terms. Purpura refers to somewhat larger areas of bleeding under the skin, while ecchymoses are what most people call bruises. So if petechiae are the tiny punctuation marks, purpura and bruises are the boldface headlines.
Petechiae Pictures: What They Usually Show
If you look up petechiae pictures online, you will usually see clusters of very small, flat dots that do not have scale, flaking, or pus. On lighter skin, they often look red, reddish-purple, or purple. On darker skin, they may appear brown, deep purple, or simply darker than the surrounding skin and can be harder to notice.
Photos of petechiae in the mouth often show tiny red spots on the roof of the mouth or inner cheeks. Skin photos often show them on the lower legs, belly, or areas that have had pressure or friction. The important visual clue is not glamour. Petechiae are not trying to win any beauty contests. They are small, flat, and stubbornly non-blanching.
Common Causes of Petechiae
1. Straining and pressure
One of the most common and least alarming causes is pressure. Hard coughing, repeated vomiting, intense crying, childbirth, or lifting something heavy can increase pressure in tiny blood vessels and cause them to leak. In these cases, petechiae often show up on the face, neck, or upper chest. They may look scary, but the story behind them is often pretty ordinary.
2. Minor injury or friction
Friction from tight straps, repetitive rubbing, sports gear, or a small injury can also lead to petechiae. Sometimes the cause is so minor that people do not remember it. That can make the spots feel mysterious when they are really just evidence of a tiny mechanical insult.
3. Medications
Certain medicines can make petechiae more likely, especially drugs that affect clotting or platelets. Blood thinners are an obvious example, but some antibiotics, antidepressants, and other medicines have also been linked to petechiae in some cases. This is one reason doctors often ask for a full medication and supplement list, including over-the-counter products.
4. Infections
Infections are a big category. Strep-related illnesses, scarlet fever, mononucleosis, cytomegalovirus, Rocky Mountain spotted fever, and other infections can be associated with petechiae. In the mouth, tiny red spots on the roof of the mouth can appear with strep infections. In severe bacterial bloodstream infections, a petechial or purpuric rash can be a medical emergency.
5. Low platelet counts and platelet disorders
Platelets are the blood cells that help your body form clots. When platelet levels are too low, or when platelets do not work the way they should, petechiae can appear. This is why petechiae often show up in discussions of thrombocytopenia and immune thrombocytopenia, also called ITP. In these situations, petechiae may be joined by easy bruising, nosebleeds, gum bleeding, or heavy menstrual bleeding.
6. Blood and bone marrow disorders
Petechiae can also occur with conditions that affect blood cell production, including some bone marrow disorders and blood cancers such as leukemia. That does not mean every tiny red dot points to a serious diagnosis, but it is part of the reason unexplained petechiae should not be shrugged off forever.
7. Blood vessel inflammation and autoimmune conditions
Vasculitis, which means inflammation in the blood vessels, can lead to petechiae or purpura. Autoimmune conditions may also affect platelets or blood vessels and create similar skin findings. When petechiae show up with joint pain, swelling, fatigue, or other systemic symptoms, doctors think more broadly than “just a skin issue.”
8. Nutritional problems and other medical causes
Vitamin C deficiency is a classic example of a nutritional cause. Aging skin and fragile blood vessels can also make bleeding under the skin more likely in some adults. In newborns, birth itself can sometimes cause petechiae, which is a very different context from unexplained spots appearing later in life.
Symptoms That May Happen Alongside Petechiae
Petechiae do not always travel alone. Depending on the cause, you may also notice:
- easy bruising
- nosebleeds
- bleeding gums
- blood in urine or stool
- heavy menstrual bleeding
- fatigue
- fever
- sore throat or swollen glands
- body aches
- shortness of breath
- weight loss or night sweats in more serious blood disorders
The bigger the symptom package, the less this looks like a harmless skin quirk and the more it looks like something worth evaluating.
When Petechiae Are an Emergency
This is the section people tend to skim, but it is the one worth reading twice. Seek urgent medical care if petechiae appear with fever, confusion, fainting, trouble breathing, a stiff neck, severe headache, rapid spreading, lethargy, or bleeding that does not stop. Petechiae with fever deserve special respect in children and adults because serious infections can sometimes present that way.
In other words, petechiae are not always an emergency, but sometimes they absolutely are. If the spots are multiplying quickly or showing up alongside signs that someone is really sick, do not play the “let’s see what tomorrow brings” game.
How Doctors Diagnose Petechiae
Diagnosis starts with context. A clinician will usually ask when the spots started, where they are located, whether they blanch, whether you have had coughing, vomiting, a recent illness, fever, new medications, unusual bruising, gum bleeding, or family history of bleeding problems.
From there, common tests may include a complete blood count to check platelet levels and other blood cells, plus a blood smear to look at cells under a microscope. If a bleeding disorder is suspected, clotting tests such as PT and PTT may be added. Depending on the bigger picture, additional evaluation may be aimed at infection, inflammation, or an immune-related cause.
The key point is that doctors are not just examining the dots. They are trying to answer the more important question: why are the dots there?
Petechiae Treatment
There is no magical “erase the dots” cream because petechiae are a sign, not a standalone disease. Treatment depends on the cause.
If the cause is minor strain or small trauma
You may not need any specific treatment beyond time, rest, and watching the area. When the bleeding is tiny and the trigger is obvious, the spots often fade on their own.
If the cause is a medication
A doctor may decide that a medicine is contributing and adjust or replace it. Do not stop prescription medications on your own, especially blood thinners or anything related to heart, seizure, or mental health care. Randomly quitting medicine is usually not a plot twist that ends well.
If the cause is an infection
Bacterial infections may need antibiotics. Viral illnesses are handled differently depending on the infection and severity. The important thing is not to assume “rash equals skin cream.” Sometimes the treatment is aimed nowhere near the skin.
If the cause is low platelets or ITP
Mild cases may only require monitoring. More significant cases can be treated with corticosteroids, immune globulin, medicines that increase platelet production, or other immune-directed therapy. In some severe or persistent situations, splenectomy may be considered. Emergency treatment may involve platelet-containing transfusions and rapid therapy for active bleeding.
If the cause is vitamin deficiency or another underlying illness
Then the fix is treating that problem directly, whether that means vitamin replacement, managing inflammation in blood vessels, or addressing a blood disorder.
Can You Treat Petechiae at Home?
Home care is only appropriate when the cause is clearly minor and there are no warning signs. Helpful steps can include rest, hydration, and avoiding additional skin trauma. Some people use a cool compress if the area is irritated. What you should not do is start guessing with random supplements or keep taking medicines that may increase bleeding without checking with a clinician.
If you have unexplained petechiae, especially if they keep returning, spread, or come with bruising or bleeding elsewhere, home treatment is not enough. That is the moment to move from internet detective to actual patient.
Petechiae in Children vs. Adults
In children, petechiae may follow crying, vomiting, viral illness, or ITP. Some children with mild platelet problems are managed with careful observation rather than immediate aggressive treatment. But petechiae plus fever, lethargy, bad headache, bloody urine, or other concerning symptoms should be treated urgently.
In adults, petechiae are often linked to medications, platelet disorders, infections, blood vessel problems, aging skin, or chronic illness. Adults may also be more likely to have a longer medication list, which makes the “what changed recently?” question extra important.
Common Experiences People Report When They First Notice Petechiae
The following examples are not individual medical records. They are realistic, experience-based scenarios that reflect how people commonly describe petechiae when they first notice them.
One very common experience starts after a rough night of coughing or vomiting. Someone looks in the mirror the next morning and sees tiny red dots around the eyes, on the cheeks, or across the upper chest. Their first thought is often allergy, irritation, or “Did I somehow get a rash overnight?” Once they learn that pressure from straining can burst tiny capillaries, the dots make more sense. In that situation, the fear usually comes first and the explanation comes later.
Another familiar story involves the lower legs. A person notices small red-brown pinpoints near the ankles or shins and cannot remember injuring the area at all. Because the spots are flat and do not itch much, they do not feel like a classic rash. That uncertainty is what bothers people. Skin problems usually come with a script: itchy, flaky, raised, irritated. Petechiae often skip that script, which makes them unsettling. Many people say the most confusing part is not pain. It is how oddly silent the spots are.
Parents often describe a different kind of panic. Their child has a fever, seems tired, and then tiny dark red dots appear. Even if the child looks mostly okay in the moment, parents can feel that the spots seem different from a routine viral rash. That instinct matters. Pediatric petechiae are not always dangerous, but they are one of those findings that can change the level of concern quickly, especially when fever or worsening illness is involved.
Some people discover petechiae during a completely different health issue. They go in for nosebleeds, heavy periods, unusual bruising, or bleeding gums and then notice the dots were part of a bigger pattern all along. Looking back, they realize the body had been dropping hints: a bruise here, gum bleeding there, tiny spots on the legs after showering. Petechiae become less of a mystery once they are seen as one clue in a larger bleeding picture.
Then there are the people who find petechiae in the mouth. They may feel a sore throat, look up, and notice tiny red spots on the roof of the mouth. That can happen with some infections, including strep-related illnesses, and it often surprises people because they did not know petechiae could show up anywhere besides the skin.
Across all these experiences, the emotional pattern is remarkably similar: first confusion, then online searching, then either relief or a very appropriate trip to a clinician. Petechiae often look tiny, but the questions they raise are not tiny at all. That is why it helps to think of them as a signal rather than a verdict.
Final Takeaway
Petechiae are tiny spots with a surprisingly wide range of meanings. Sometimes they are the harmless result of pressure from coughing, vomiting, or minor trauma. Sometimes they are a clue to low platelets, medication effects, infection, inflammation, or another underlying medical problem. The appearance matters, but the context matters more.
If petechiae show up once after obvious straining and then fade, the story may be simple. If they appear without a clear reason, keep returning, spread, or come with fever, unusual bruising, bleeding, or signs of serious illness, they deserve medical attention. Tiny spots can carry big information. Your job is not to diagnose them from across the bathroom sink. Your job is to notice them, take them seriously, and know when to get help.